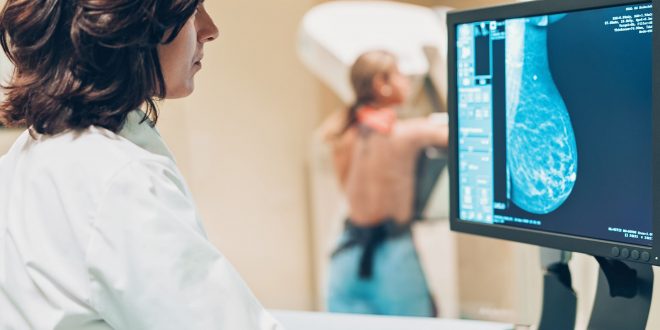
Over the last 30 years, mammography has been used to detect breast cancer in various countries, initially using analog screen-film-based technologies and then switching to fully digital technologies over the last 20 years.
Since the dawn of digitization, computer-aided detection (CADe) and diagnosis (CADx) algorithms have been a subject of intense interest, which has led to the development of computer-aided interpretation.
Despite the high expectations, the positive impact that these systems could have on the clinical community failed to materialize, primarily due to high false-positive rates per image.
Digital mammography and breast tomosynthesis have adopted an artificial intelligence (AI) approach by using deep learning.
And convolutional neural networks to detect and diagnose breast cancer in the last five years.
It was first studied concerning conventional CADe/CADx methods to determine how this new technology compared, which quickly showed its potential.
In retrospective analyses, comparisons of algorithms developed in the last few years with those conducted by experienced breast radiologists demonstrate that these algorithms perform as well as their human counterparts.
It is becoming clear that artificial intelligence will have an essential role in screening breast cancer in the future, despite additional studies, especially those done in the real screening environment.
Although there is still much uncertainty about how this new player will affect the marketplace, recent studies have taken a look at different methods for implementing this technology.
This review uses digital mammography and breast tomosynthesis to introduce viewers to the basic concepts and advances in artificial intelligence for breast cancer detection.
It will be discussed how conventional methods are prone to pitfalls and how this new approach avoids them largely.
The presentation will discuss recent studies investigating how AI and machine learning can improve medical practice and ask the questions that need to be addressed before this vision can occur.
Breast cancer screening and detection
Breast cancer kills over half a million women around the world every year.
Over the past three decades, mammography has been used in many countries worldwide to reduce mortality from breast cancer.
As a result of screening and treatment improvements, breast cancer death has decreased by 30%, but it remains the leading cause of cancer death for women.
Across the world, mammography screenings for breast cancer are implemented differently. Most countries, such as the US, screen their citizens via institutions.
Women go to a breast imaging center, associated with an area hospital or often found in a primary care physician’s office or gynecologist’s office, for a breast cancer screening by themselves.
The individual institution determines screening details, such as the manufacturer and tomosynthesis software, even though digital mammography and digital breast tomosynthesis are heavily regulated.
As long as the woman waits to be seen, the images could be interpreted during her consultation, and any additional imaging could be done on the same day.
One or two days after acquisition, the screening exams are read in batches at larger screening centers, and if there is something suspicious found, the woman needs to be recalled.
You May Like Also: AI Apps for the Alzheimer’s Prediction
Particularly in Europe, the government (regional or national) has implemented breast cancer screening programs widely.
Usually, women between 50 and 70 years of age are invited to participate in such a program for a mammogram screening every two years.
Some screening programs operate their dedicated screening centers independent of hospitals.
A large or complete degree of homogeneity is evident in such a program.
Referrals to hospitals are usually recalled since examinations are batch-read and then forwarded to them for further imaging and testing.
Mammographic screenings are meant to identify lesions with two distinct characteristics. A calcification cluster is a complex tissue lesion; a soft tissue lesion is a calcification cluster.
As little as 0.2 mm of calcification is interesting for detecting breast cancer, which is relatively high in contrast.
Physiopathology and radiology both use calcification distribution and shape as biomarkers to identify malignancy.
Lesions of soft tissues and fibroglandular tissue are noted: smooth, obscured, irregular shapes and patterns and asymmetries in dense tissue patterns at one breast that do not correspond to lesions on the contralateral breast.
Breast cancer is detected by detecting changes in the finding, on average growth, as one of the significant biomarkers.
It is generally considered to be unimportant if a suspicious finding is found to not change over time.
Previous images should be compared in the interpretation of screening mammography images, as this can increase sensitivity and specificity and provide additional information not available from other concurrent imaging techniques, such as Digital Breast Tomography.
Each case is usually double read in many screening programs, especially in Europe.
According to the reader, the images have been interpreted as a referral to evaluate the suspicious finding further.
If two radiologists disagree with their assessment in the program, they can either meet in person to resolve the dispute or bring a third expert radiologist into the discussion.
It has been shown that double reading has a positive predictive value, although it requires more resources than the standard single reading screening process in the US.
The recall rate, in other words, the percentage of screened women who are recalled or referred for further testing, is another significant difference between screening in Europe and the US.
For example, the referral rate in Amsterdam and Sweden is about 2.5 %, and the recall rate in the US today is 11.5 % *30 % lower because of DBT.
Different practices and the medico-legal consequences of misses may account for the difference.
If a woman is recalled or referred following the screening, she is then evaluated for a lesion of concern by a diagnostic work-up.
A breast ultrasound or MRI, along with DM and DBT imaging, may be required as part of this work-up.
An interpreting radiologist evaluates the additional imaging findings to determine whether or not a biopsy is necessary.
In rare cases, a biopsy might be performed using an excisional biopsy technique. This procedure depends on the type of lesion and can be performed using fine-needle aspiration, core, or vacuum-assisted biopsy.
Depending on the outcome of the screening assessment, a true positive or false positive diagnosis can be reached based on the pathological analysis of the biopsy-obtained sample.
And, depending on whether or not she was diagnosed with breast cancer during the period between screening rounds, guidelines may deem this a false negative if the screening was assessed as usual.
Digital mammography
Screen-film mammography was initially used as a screening method for breast cancer.
Digital mammography (DM) was created and introduced for medical use in the early 2000s when large-area digital detectors became affordable.
A digital detector instead of the film was used in DM, producing an instant digital image, which the acquiring radiographer and the radiologist could use to evaluate the image and determine if it was valid.
Mammography produced using computed radiography can serve as an intermediate path to the digitization of breast screening.
This technology has been shown to perform poorly in various studies, and therefore its use is declining.
Mammography by DM, on the other hand, is much simpler than by screen-film mammography.
DM has improved clinical performance compared to screen-film mammography in subgroups of the screening population, but in general, DM has the same performance as screen-film mammography.
A further advantage of digital detectors for imaging the breast is that more advanced methods for acquiring and processing images,
Such as digital breast tomography and dedicated breast computed tomography, as well as algorithms for post-acquisition analysis and reconstruction, can now be developed quickly.
Regardless of the technology used, a two-dimensional breast image is acquired through traditional film and digital mammography.
There is a phenomenon known as tissue superposition, in which different breast tissues, separated only by their projection directions, are projected on the exact location during a 2D mammogram.
Isolated normal tissues can mimic suspicious lesions, reducing specificity, and the presence of normal tissues may disguise a malignant lesion, reducing sensitivity.
When a breast has sizable fibroglandular tissue, these effects can significantly reduce mammography’s accuracy.
One-third of all cancers missed are caused by this mutation, which occurs in half of the screened breasts.
Two breast views are acquired for screening mammography using two different views: the craniocaudal (CC) and middle lateral oblique (MLO) views. This alleviates the issue of tissue superposition and loss of performance in dense breasts.
Radiology interpretation is a cognitive process in which interpreting radiologists assemble both images simultaneously to determine whether a lesion seen on one view is also present on the other,
The extra breast tissue can be discarded or superimposed on the other views hoping that another breast compression direction will reveal an otherwise occult lesion.
In summary, screening mammography interpretation involves analyzing and comparing features or the absence thereof among two images taken simultaneously and across two pictures taken at two different time points.
It would be ideal for any algorithm to detect breast cancer at the screening to make these exact comparisons to maximize performance.
Digital breast tomosynthesis
Because of limitations in DM as a two-dimensional imaging method, digital breast tomosynthesis has developed and been clinically introduced over the past two decades.
Using DBT, pseudo-tomographic images of breasts are generated as a stack of 2D slices, with some vertical resolution, although limited.
In this case, the effect of the partial tomography is to reduce the masking impact of the superimposed tissues.
The results of trials on DBT for cancer detection at screening have been promising, but DM has the advantage of a shorter interpretation period.
Inconsistent reports, the interpretation of DBT images requires approximately twice as much time as reading DM images due to many images to be reviewed.
The adoption of DBT in large-scale screening programs will also hinge on reducing the amount of time it takes to read texts and its impact on clinical outcomes.
An automated interpretation of these images will likely have a bearing on using DBT as a screening tool.
The impact of this is twofold: First, computerized, faster navigation of images from the DBT stack may significantly reduce the amount of time that a radiologist spends searching for suspicious photos.
Further, suppose the inter-reader variance is reduced by using computational methods to aid in interpreting DBT images. In that case, one may see less variability across studies concerning the impact of DBT on screening recall rates.
What is the process by which AI detects breast cancer?
MammoScreen, an AI algorithm that can identify suspicious areas on a digital mammogram and decide whether they are likely to be cancerous, was used by researchers.
A total of 4 views of the mammogram are taken into account, as well as a score for suspicion of malignancy.
How does artificial intelligence treat breast cancer?
AI can help determine what order mammograms should be reviewed by the physician based on the results of the AI tool. An immediate review of the mammogram may be required if the AI tool identifies areas suspicious for cancer on the patient’s mammogram.
Mammography AI: what does it mean?
It exists for both digital mammography, digital breast tomosynthesis, and full-field digital mammography FFDM. An AI program can identify and predict malignant features in images and use the information to aid in clinical diagnosis.
AI in the detection of cancer: how does it work?
Both of these benefits can be gained by utilizing artificial intelligence systems, which can help by reducing the burden on specialized specialists and detect lung spots invisible to the naked eye. Malignant tumors are closely monitored by radiologists using a variety of computer-aided diagnostic tools.
What is the most effective way to detect breast cancer?
It is only through a biopsy that breast cancer can be definitively diagnosed. An imaging test or an x-ray is used to guide your doctor in extracting tissue samples from the suspected area during a biopsy.
 Next Tech Magazine Get The Latest Technology Updates
Next Tech Magazine Get The Latest Technology Updates